Life After Cancer Treatment: Why Nobody Warns You About This Part
Nobody tells you about the quiet that comes after.
They prepare you, as much as anyone can, for the hard parts of cancer treatment. The chemotherapy, the hair loss, the nausea that doesn’t quit, the port they install in your chest so they can poison you on a schedule. They tell you it will be hard and they tell you to stay strong and they tell you how brave you are. And you smile and you say thank you and somewhere inside you think, I don’t actually have a choice here. What exactly would the alternative look like?
What nobody talks about is what happens when life after cancer treatment begins. When the last IV drips through and the bell rings in the chemo ward and you walk out to the parking lot and realize that the entire structure that has organized your life for the past year is suddenly just gone. No more weekly nurse calls. No more symptom journals. No more appointments circled on the calendar every few weeks. Just you, standing in the parking lot, full of poison for the last time, trying to figure out how to start looking outward again when your whole self has been pointed inward for so long.
That transition is what nobody prepares you for. And it is harder than most people expect.
The Bell

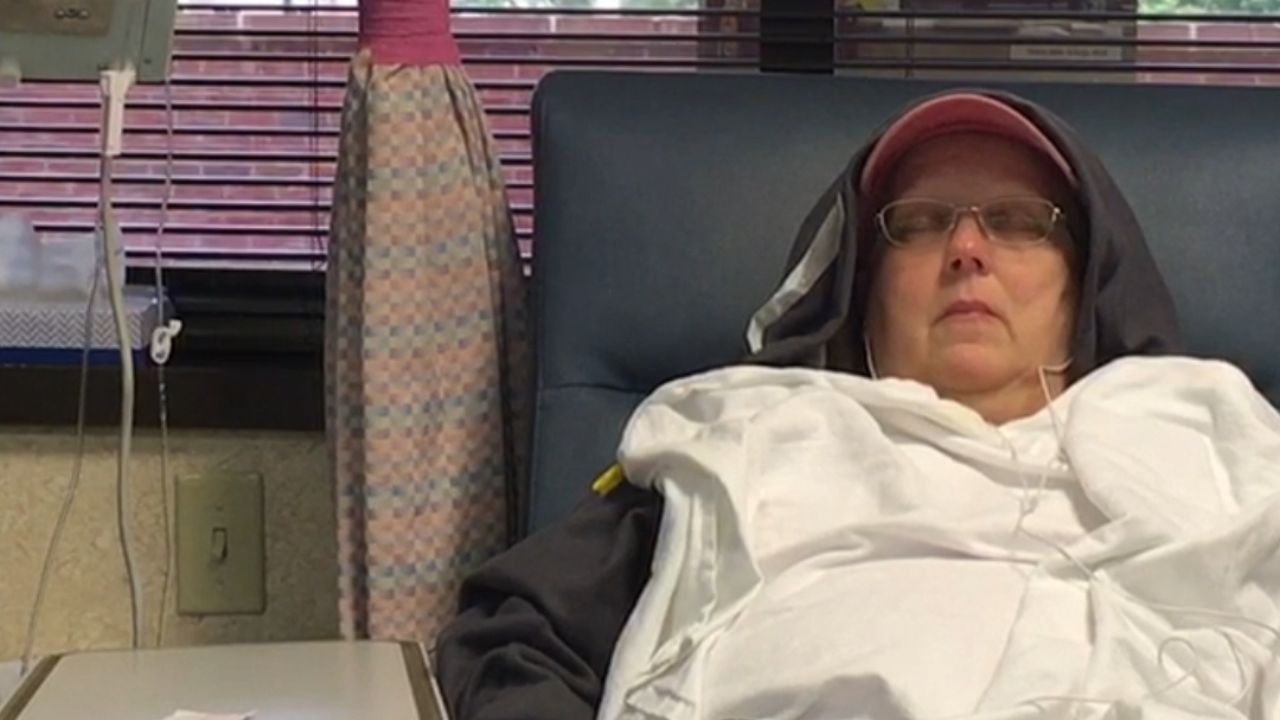
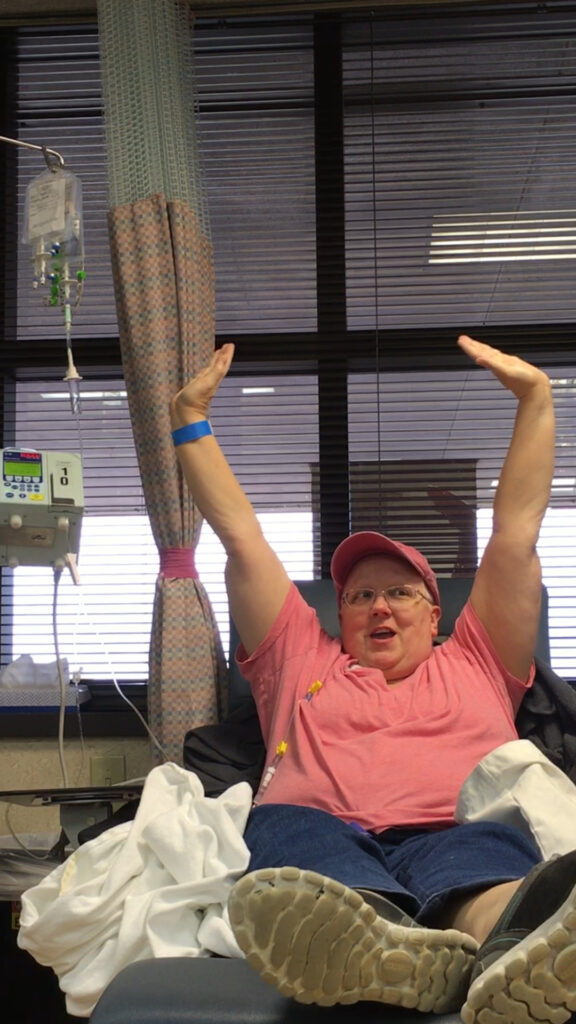
In August 2017 I sat in a chemo chair and watched the last bag drip through my port for the sixteenth and final time. That is the photo at the top of this page.
There is a bell in the chemo ward. You ring it when your last treatment finishes. It is a small ceremony, a moment of acknowledgment from the nurses and the other patients in the room, and I rang it while simultaneously not wanting anyone to look at me, which is a very specific kind of contradictory feeling. I have photos. I have a video. I was relieved and exhausted and already thinking about the fact that the stacking debuff could finally start to unwind.
If you have ever played a video game where negative effects accumulate on your character, you have a rough idea of what sixteen rounds of chemotherapy feels like from the inside. Every treatment adds another layer of toxicity on top of the last. You don’t recover between rounds, you just add more on top of what’s already there. My body had been running that way for five months, and from this point forward, the poisoning was done and the healing could begin.
That part, I was ready for.
What I was not ready for was the sudden silence where the medical structure used to be.
The Weekly Call That Stopped
During treatment I had a system, and that system gave me something to hold onto. Every week a nurse called to check on me. I kept a running list of symptoms and changes to report on each treatment day. I saw my oncologist regularly and knew that someone was always tracking how I was doing. My entire mental and physical energy was organized around a simple loop: notice, record, report.
When chemo ended and surgical recovery began, the oncologist stepped back. No more weekly calls. No more symptom tracking with someone waiting on the other end to receive the information. A follow up appointment in roughly two months, and in the meantime, just silence.
Two months of silence after nearly a year of constant monitoring is a very strange thing to navigate. My brain had been trained to scan constantly, to pay attention to every sensation and ask the same question about every twinge and ache. And that question does not turn off simply because treatment ends. If anything it gets louder, because now your body is full of new post-surgical pain that is harder to interpret. The implant settling into place. The cadaver skin they use in reconstruction pulling everything tight across your chest. The pec muscle, which you did not previously know you had, now flexing in unfamiliar ways that hurt every time you move your arm a certain direction. Nerves that were cut during surgery slowly waking back up and sending electric zaps through your chest at random moments throughout the day.
And underneath every single one of those new sensations, the same question that was already living in the back of your mind. Is this the cancer coming back?
I kept tracking symptoms anyway, just for myself, because knowing I could call the oncologist’s office if something felt genuinely wrong gave me enough of a safety net to function. But the external structure of being monitored was gone, and I had to learn to carry that vigilance on my own.
Nine years later, I still feel it. A dull ache near my gallbladder and the first thought is always, is this my liver? Is something spreading? You learn to talk yourself down from it, to remind yourself that not every physical sensation is a crisis, and you genuinely come to believe it over time. Because here is the thing that never stops being true: the human body is extraordinary. It can be poisoned on purpose, repeatedly, cut open and reconstructed, and it will immediately begin trying to heal itself. That is remarkable. I never stop being grateful for it.
But the question never fully goes away. You just get better at living alongside it.
What Everyone Gets Wrong About Strength
During the treatment year, people told me constantly how strong I was. How amazed they were by my attitude. How brave I seemed.
And I would smile and say thank you and think, privately, that I had absolutely no other choice.
Strength implies you could have chosen something different. That there was a softer path available and you decided to take the harder one. There wasn’t. There was just the next necessary thing, and then the thing after that, and the thing after that. The world outside kept moving, politics and grocery shopping and other people’s ordinary concerns, and none of it registered because my entire existence had narrowed down to one question: am I going to be okay?

That narrowing is what survival mode actually feels like from the inside. It is efficient and it is necessary and it kept me functional for an entire year of hard things. But what I didn’t understand until much later is that survival mode doesn’t automatically disengage when treatment ends. You have to learn, consciously and sometimes painfully, how to widen back out. How to let the world back in. How to start asking different questions.
That process took me a lot longer than I expected.
The Long Unwinding
Treatment ended in late 2017. My father had died seven months before my diagnosis, from lymphoma. My mother died in 2019. Then in 2022 and 2023, three of my four cats died within a single year.
Loss kept stacking long after the chemo stopped.
I stepped back from my knitting livestreaming. I stopped uploading to my knitting YouTube channel, the one I had built over years and streamed through my entire treatment. The community that had been with me through everything was still there, but I simply could not show up for it anymore. The knitting itself had gotten tangled up in my mind with the exhaustion of treatment and the grief of that year, and I needed to separate those things before I could find my way back to it. I was worn down in a way that felt total, and I knew I didn’t want to keep living that way, but knowing it and having the energy to do something about it are very different things.
It was water that started to bring me back.
About two years after my surgery, I got back into the pool for the first time. My chest muscles had been pulling tight ever since the reconstruction, drawing my shoulders inward, keeping everything contracted. When I got into the water and started moving my arms and stretching those muscles against the resistance of the water, something let go. I cried right there in the pool, which sounds dramatic but wasn’t, it was just my body releasing something it had been holding for a very long time. That stretch, that opening, was something I had needed without knowing how badly I needed it, and the water gave it to me.

I wanted more of that feeling.
I started swimming regularly, almost daily. I started looking for moving water, lazy rivers where I could be weightless and carried by a current, feeling the cold water against my skin and the particular kind of freedom that comes from floating. There are several hotels in my city that offer a day pass to use their pools, and they both had a slow lazy river. Perfect! My sister and I went several times and just had the time of our lives floating around those circuits. I wanted more, then I found the fast lazy river at Aquatica and it was perfect: fast enough to feel like a real current, strong enough to work your body, cold and refreshing and just the right amount of challenging. Went a handful of times and I wanted more. I next found Universal’s Volcano Bay to try their version. Their river releases massive waves that hit you and then bounce back from the wall and hit you again, and staying upright requires real effort. It was less lazy river and more survival situation. Fun, technically, but not what I was looking for. I didn’t need more anymore, Aquatica was exactly right.
There is actual science behind why moving water heals the way it does. The hydrostatic pressure improves circulation. The buoyancy takes weight off your joints. The flowing water acts as natural white noise that calms the nervous system and lowers cortisol. The rhythm of it helps release emotional stagnation. I did not know any of that when I first got into the pool. I just knew that my chest opened up and I cried and I wanted to feel that again.
While I was finding my way back to my body through water, I was also learning digital marketing. I took a course, got into the software, became excited about funnels and affiliate programs and the idea of building an income online. I told everyone I knew about it. My friends and family listened politely and then said, almost unanimously: go back to knitting. You are good at it. You enjoyed it. You made money from it before. Why are you trying to sell a course?
They were right, and I knew it, but I wasn’t ready yet. The knitting was still tangled up with everything else. The livestreaming burnout. The exhaustion of streaming through treatment while conversations with chatters sometimes brought me their heaviest problems because I had become a safe place for them. The grief of stepping away from a community that had been with me through the hardest year of my life.
I had to grieve the version of myself that used to show up every day and teach knitting on the internet before I could figure out what the next version looked like.
So I took everything I had learned about digital marketing and I applied it to knitting. Years ago, I had started a knitting YouTube channel that I had neglected and began uploading knitting tutorials again. I launched a blog about knitting. I created a free knitting pattern and began an email list. I built automated systems so my new friends get emails from me regularly. I applied for the Amazon Influencer Program, and started filming shoppable product videos from items around my house. These videos appear on Amazon’s product pages, and now I am making a steady income. I started this blog offering my opinions about the products I use and exploring the Life after 50 experiences I’ve been living. For the first time in a very long time, I feel like I’m moving forward.
The friends who told me to go back to knitting were right. But I had to find my way there in my own time, which meant first learning something new and then using it to come home.
Scan Months
For eight years, March and September were my scan months.
Every March and September I had oncology appointments, cancer bloodwork reviews, mammograms, chest x-rays, ultrasounds, and a breast MRI every September. An entire infrastructure built around watching for the thing that had already tried to take me once. I moved through those months and then deliberately set the whole thing aside until the next time, because the only way to live in between, was to not let the watching consume everything.
Last year, my family doctor flagged some concerning numbers in routine bloodwork. My hematocrit, hemoglobin, and red blood cell count were all running high, which can sometimes indicate a condition called Polycythemia Vera, a bone marrow disorder that causes overproduction of red blood cells and carries its own cancer-related concerns. I tend to run high as a general rule, and dehydration can be a factor, but she wanted to rule it out and sent me back to the oncologist for additional bloodwork.
When she said the word oncologist, it ricocheted through every part of my body.
Not the drive over. Not the waiting room. That word, in that moment, in my family doctor’s office, and every fear I had ever carried about cancer coming back moved through me all at once. Eight years of scan months. Eight years of that question living in the back of my mind. And there it was again, summoned by a single word in an ordinary appointment.
I had to go. More bloodwork, more waiting, more sitting with the not knowing. The oncologist ran the tests and told me everything was okay.
But I want to be honest about what that moment felt like, because I think a lot of people who have been through treatment know exactly what I am describing and nobody talks about it. You do not get to a place where the fear is gone. You get to a place where you have learned to keep moving while it is present.
What Surviving and Living Actually Feel Like
I have been thinking a lot lately about the difference between the two, and I think the clearest way I can explain it is this.
Surviving is the year of treatment when your whole self narrows down to one question and you do the next necessary thing because you have no other option. There is no bandwidth for processing fear or grief or trauma during that year. You just do it. I’ve recently been reviewing past knitting livestreams pulling out nuggets that I can share with my knitting audience and I am watching myself through the various phases of cancer treatment. When I first showed up on stream with a bald head, I joked that when I look in the mirror I wondered what is Captain Picard doing here? Several months later, as my hair started to grow again and I was proud of my 1/4 inch locks, a viewer asked how I identified. I removed my ball cap and said today I identify as a grandpa. And I looked every inch of an old man with thin gray hair, tired and worn out.

Living is what comes after, and it is not a destination you arrive at cleanly. It is the long unwinding. It is water opening up your chest in a pool and crying because you needed that stretch for two years and didn’t know it. It is separating the grief of burnout from the joy of knitting and finding your way back to something you love on your own terms. It is coming to terms with your body and how different it feels and looks. It is learning new things because curiosity means you are reaching toward a future. It is the oncologist word ricocheting through your body in a doctor’s office and going anyway and getting the all clear and going home and making dinner.
And it is grief, still. I recently lost another cat. After everything, after all the loss that has stacked up over these years, I sat with this one, as I had with the others, as he crossed over I felt it fully. The tears came. They are coming now as I write this. But something is different this time. I am moving through it rather than being flattened by it. I am aware of the sadness and I am not trying to push it away, but I am also keeping my eye toward what comes next. I was with him through all of it. I helped him go peacefully. I am still here. I am okay.
That shift, from being consumed by grief to being able to hold it and keep going, is not something I could have done at the beginning of this. It is something I learned slowly, through years of practice, through water and movement and building things and allowing the late-arriving emotions from treatment to move through me when they surface.
Living is understanding that the processing never fully ends. It just gets more manageable. You get more centered. You learn to feel the thing without drowning in it.
If You Are In the Quiet Part Right Now
If you just finished treatment and you are sitting in the strange silence where the structure used to be, I want you to know that what you are feeling makes complete sense.
Your brain has been organized around survival for months. The monitoring has stepped back. The world is asking you to return to normal and normal doesn’t feel like anything you recognize anymore. The grief and fear and trauma that had no bandwidth during treatment are starting to surface now that there is finally space for them, and that is disorienting and exhausting even when you are technically done with the hard part.
Give yourself the time. Let the processing happen in whatever order it arrives. Be patient with the emotions that show up late. Find your water, whatever that is for you, the thing that opens your body back up and reminds you what it feels like to be weightless and present and not just enduring.
And know that the distance between surviving and living is not crossed in a single moment. It is accumulated in small things over time. A stretch in a pool that makes you cry. A friend telling you to go back to knitting. An ordinary appointment where a word ricochets through you and you go anyway and come home okay.
You will get there. Not all at once, and not on anyone else’s timeline. But you will get there.

Want to read more of my discoveries at Life After 50? Read my article: Just the Next Hard Thing: My Mastectomy Recovery Story or After Cancer, I Needed Something to Do With My Hands